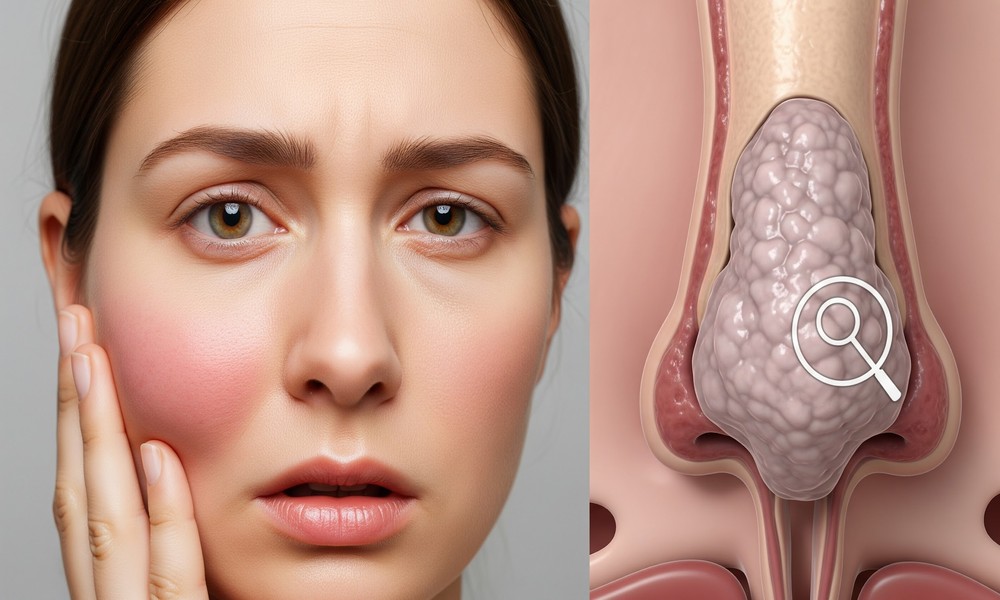
Facial swelling and nasal congestion are common complaints, often linked to allergies, sinus infections, or minor injuries. In most cases, these symptoms resolve with routine care and time. However, when swelling persists, worsens, or presents alongside unusual changes, it may signal something more complex occurring beneath the surface.
Rare cancers affecting soft tissue in the head and neck region can initially mimic benign ENT conditions. Because these cancers often develop quietly and progress gradually, early symptoms may be overlooked or attributed to more common explanations. Understanding when facial swelling or nasal masses require deeper evaluation is essential for timely diagnosis and appropriate care.
Common Causes of Facial Swelling and Nasal Obstruction
Facial swelling and nasal blockage frequently arise from inflammation. Sinus infections, allergic reactions, dental issues, and trauma can all cause tissue irritation and fluid buildup. These conditions are usually accompanied by pain, pressure, discharge, or fever, and they often respond to medication or supportive care.
Structural issues may also contribute. Deviated septums, nasal polyps, or chronic sinus disease can cause ongoing congestion or asymmetry in facial appearance. These issues tend to develop gradually and may fluctuate over time, often improving temporarily with treatment.
Because these explanations are so common, persistent or progressive swelling may initially be dismissed. This makes it especially important to recognize patterns that do not follow the expected course of routine ENT conditions.
The Role of ENT Evaluation in Early Detection
ENT specialists play a crucial role in distinguishing routine conditions from those requiring advanced care. Through physical examination, nasal endoscopy, and imaging, they can assess whether swelling originates from mucosal inflammation, bone structures, or soft tissue masses.
In healthcare settings, such as Kimball Health Services, ENT care often involves evaluating persistent nasal masses and coordinating further diagnostic testing when tumors are suspected. ENT providers are frequently the first clinicians to identify abnormal growth patterns in the nasal cavity or facial structures.
Early identification at this stage can significantly affect outcomes, especially when rare cancers are involved.
Red Flags That Warrant Further Investigation
While most facial and nasal symptoms are benign, certain warning signs suggest the need for additional evaluation. Swelling that does not respond to antibiotics or allergy treatment, nasal obstruction on one side only, or unexplained facial asymmetry should prompt closer attention.
Other concerning features include numbness, unexplained bleeding, pain that radiates to the eye or jaw, changes in vision, or a mass that continues to enlarge over time. These symptoms may indicate deeper tissue involvement rather than surface-level inflammation.
In such cases, imaging studies and specialist evaluations are often necessary to determine whether the cause is inflammatory, structural, or something more serious.
Understanding Soft Tissue Sarcomas of the Head and Neck
Soft tissue sarcomas are rare cancers that originate from connective tissues, including muscle, fat, nerves, and blood vessels. When they develop in the head and neck region, they may present as painless swelling, nasal blockage, or facial distortion rather than classic cancer symptoms.
Because these tumors can grow in confined anatomical spaces, even small masses may cause noticeable functional changes. Pressure on nerves, sinuses, or ocular structures can lead to symptoms affecting vision, breathing, or sensation.
Specialized centers such as the Sarcoma Oncology Center, which focuses on soft tissue sarcoma treatment and head and neck sarcoma, are often involved once imaging or biopsy suggests a malignant process. These centers coordinate advanced diagnostics and treatment planning tailored to rare cancer types.
Imaging, Biopsy, and Diagnostic Challenges
Diagnosing rare head and neck sarcomas requires careful interpretation of imaging and tissue samples. CT scans and MRIs help determine the size, location, and extent of a mass, but imaging alone cannot confirm cancer type.
Biopsy is essential, yet obtaining tissue from delicate facial or nasal areas must be done carefully to avoid complications. Pathologists with experience in sarcoma diagnosis play a critical role, as these tumors can resemble benign growths under initial examination.
The diagnostic process may take time, but accuracy is critical. A precise diagnosis informs treatment planning and reduces the risk of incomplete or inappropriate intervention.
Surgical Considerations in Facial and Nasal Tumors
When tumors affect the face or nasal structures, surgery often involves both cancer removal and preservation of function. The goal is to eliminate malignant tissue while maintaining breathing, vision, speech, and appearance whenever possible.
Facial reconstruction may be required following tumor removal. Specialists such as those at North Texas Facial Plastic Surgery, where facial plastic surgeons in North Texas focus on facial reconstruction, contribute expertise in restoring structure and symmetry after complex resections.
This collaborative approach helps address both medical and quality-of-life concerns, recognizing that recovery extends beyond disease control alone.
Coordinated Oncology Care and Long-Term Monitoring
Treatment for soft tissue sarcoma may include surgery, radiation, chemotherapy, or a combination of approaches, depending on tumor type and stage. Because these cancers are rare, treatment plans are often individualized and guided by multidisciplinary teams.
Centers like the Sarcoma Oncology Center emphasize coordinated care that integrates oncology, surgical planning, imaging, and long-term surveillance. Monitoring after treatment is essential, as sarcomas can recur locally or spread to other areas.
Ongoing follow-up allows clinicians to address late effects of treatment, manage functional changes, and support patients through survivorship.
Emotional and Functional Impact of Facial Tumors
Beyond physical symptoms, facial and nasal tumors can profoundly affect emotional well-being. Changes in appearance, breathing, or sensory function may influence self-image, communication, and daily activities.
Patients often face uncertainty during diagnosis and treatment, especially when symptoms were initially subtle or misunderstood. Access to supportive care and clear communication helps individuals navigate these challenges more effectively.
Recognizing the emotional dimension of facial cancers reinforces the importance of comprehensive care that addresses both physical and psychological needs.
Conclusion: Listening to Persistent Symptoms
Facial swelling and nasal masses are usually harmless, but when symptoms persist, progress, or defy standard treatment, they deserve careful evaluation. Rare cancers such as soft tissue sarcomas can present quietly, making early recognition essential.
By understanding warning signs, seeking timely ENT assessment, and pursuing appropriate diagnostic pathways, patients and clinicians can work together to identify serious conditions sooner. A coordinated approach that integrates medical expertise, surgical planning, and long-term support offers the best opportunity for effective treatment and preserved quality of life.